The United States federal government spent $3.2 trillion in healthcare, which is about $9,900 per person, in 2015. This figure accounts for 17.8% of the GDP and is expected to increase annually by almost 6%. [1] According to WHO, the United States also spent around 17.1% of its GDP in healthcare in 2014, which is significantly higher than Sweden’s 11.9% and Switzerland’s 11.7%. Other developed countries like Canada and Japan only spends about 10% of their GDP in healthcare. [2] The US government aims to reduce their spending by integrating new technologies like telemedicine into healthcare.
In a recent blogpost that we published, we looked into some of the major challenges to adoption of telemedicine.
Defined as the remote delivery of healthcare using telecommunications technology for diagnosis, treatment, disease prevention, and care management, telemedicine makes accessible, convenient, and cheaper patient care possible. Through telemedicine, medical professionals can now look after patients with urgent needs using remote devices. Rehabilitation and disease interventions can be done in the comfort of a patient’s home, instead of being performed through costly hospitalizations. With telemedicine, doctor shortages in small community hospitals and in rural areas may soon be a problem of the past.
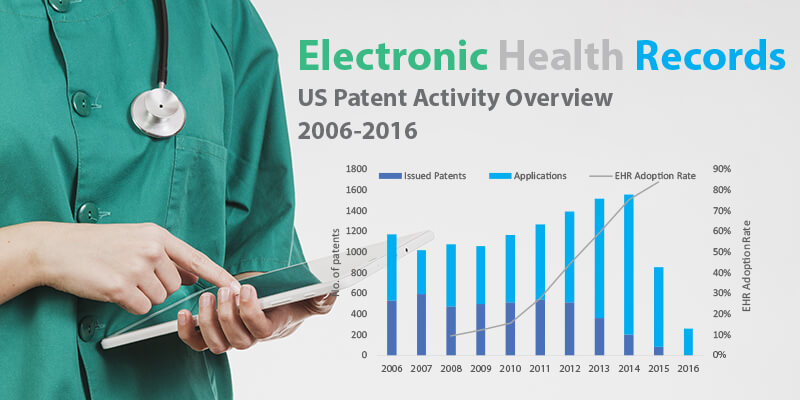
At Parola Analytics, we look at telemedicine patents to get a glimpse of how companies and innovators are shaping the future of the technology. US patent data over the last ten years shows that an increasing number of patents related to telemedicine are being filed at average growth rate of 8%. In 2016, there were 243 patents filed in the US while 159 patents were filed in 2007.
Various pieces of legislation have been put in place by the federal government to demonstrate support towards telemedicine’s implementation. The Medicare Telehealth Parity Act was signed into law in 2014, expanding telehealth coverage under the Medicare program. [3] The following year, an updated Medicare Telehealth Parity Act of 2015, which includes more services and removes geographic barriers to telehealth services, was introduced in the House but was not enacted.
The Expanding Capacity of Health Outcomes Act (ECHO Act) was also passed in 2016. The law requires the Department of Human Health Services to conduct studies examining technology-enabled learning and capacity building models. The aim is to expand use of healthcare technology to reach out to rural communities and serve populations in need of critical health services. [4] The government also enacted the 21st Century Cures Act – promising increased access of Medicare beneficiaries to telehealth services. [5]
At the state level, a growing number of states have also shown support for the implementation of telemedicine. One of the pioneer states to show support was California, where the Telehealth Advancement Act was signed into law. This law lifted the ban on electronic remote care services, which allows health professionals to be telehealth providers. [6] The last state to scrap the law requiring in person visit prior to using telemedicine, Texas, has recently passed Bill 1107. The passage of this bill expands the use and eases the restrictive access of telemedicine in Texas. With this, all 50 states now allow direct-to-consumer telemedicine companies to operate video-based telemedicine solutions. [7,8]
As for reimbursement policies, all states offer coverage except for Connecticut and Rhode Island. However, laws and policies for telemedicine reimbursement under Medicaid differ across states, according to a report by the Center for Connected Health Policy. Many states have expanded telemedicine reimbursement benefits, while some still limit the delivery of telemedicine services. Only nine states reimburse all three telemedicine services -live video, remote monitoring, store and forward – under Medicaid: Alaska, Arizona, Hawaii, Illinois, Minnesota, Mississippi, Missouri, Virginia and Washington. [9]
There are also limitations to what can be reimbursed under store and forward and remote monitoring and live video modalities. Forty-eight states and Washington DC implemented policies in telemedicine reimbursements for live video services but restrictions still apply. Some states only offer reimbursements for certain medical specialties, types of services, types of providers, and locations. For example, New Jersey only reimburses telepsychiatry services. Thirteen states have Medicaid programs which reimburse store and forward services, while 22 states only reimburse remote patient monitoring. [9]
There are also telehealth parity laws requiring private payers like insurance companies to cover and reimburse telemedicine services like in-person visits. This is essential to ensure accessible and low-cost telemedicine services. Over 29 states have telemedicine parity laws and eight states have proposed parity laws. [9] Licensing of telemedicine services in several states is burdensome and limit growth across states.
Different telemedicine and medical practice laws and standards in different states make it difficult to develop a uniform framework. For telemedicine companies to scale, regulatory frameworks allowing them to operate across state borders need to be harmonized and put in place. Conflicting definitions and differences in regulation also create confusion for telemedicine participants, especially when providers and practitioners offer services in multiple states. [8] Health plans may not cover all the services the telemedicine provider is offering, which may lead to uncertain reimbursements.
There are also differences in policies regarding consent, licensure, online prescription, and private payers. Medical malpractice and liability issues regarding telemedicine are also uncertain in some states, leaving medical providers clueless about legal obligations and responsibility. [10] These regulatory challenges need to be overcome for the full implementation of telemedicine nationwide.
But amidst these difficulties, growth in the telemedicine market is undeniable as more hospitals opt to include telemedicine in their services. Telemedicine may soon become an integral part of healthcare. Telemedicine solutions are not just limited to home healthcare delivery but is also seen to expand to areas such as disease management, disaster preparedness and response, and clinical decision support.
Read more on Telemedicine here.
[10] With telemedicine’s potential, it is crucial for policymakers to study the regulatory and organizational issues inhibiting its adoption for this life-saving solution to fully take off.
[1] “NHE-Fact-Sheet.” Centers for Medicare & Medicaid Services. N.p., 21 Mar. 2017. Web. 23 Mar. 2017.
[2] World Development Indicators | The World Bank. N.p., n.d. Web. 07 June 2017.
[3] Lacktman, Nathaniel, “Five forces driving telemedicine expansion in 2016,” Managed Healthcare Executive, 11 Feb 2016. Web. 22 Dec 2016.
[4] Office of the Press Secretary, “Statement by the Press Secretary on H.R. 3471, H.R. 4419, H.R. 5111, H.R. 5509, H.R. 5995, S. 795, S. 817, S. 818, S. 1550, S. 1555, S. 1632, S. 1808, S. 1915, S. 2234, S. 2873, S. 2974, S. 3028, S. 3076, S. 3183, S. 3395, S. 3492,” The White House, 14 Dec 2016. Web. 22 Dec 2016.
[5] McCArthy, Jack. “21st Century Cures Act a boon to telehealth, experts say.” Healthcare IT News. N.p., 16 Dec. 2016. Web. 04 Apr. 2017.
[6] “Telehealth Advancement Act.” CCHP. N.p., n.d. Web. 04 Apr. 2017.
[7] Mazur, Lisa, and Ryan Marcus. “Last but Not Least, Texas Takes the Final Steps to Embrace Telemedicine.” The National Law Review. N.p., 24 May 2017. Web. 30 May 2017.
[8] Comstack, Jonah. “In-Depth: What Texas’s landmark telemedicine legislation means for the industry and the nation.” Assurgent. N.p., 26 May 2017. Web. 02 June 2017.
[9] State Telehealth Laws and Medicaid Program Policies A Comprehensive Scan of the 50 States and District of Columbia. Rep. N.p.: n.p., n.d. Center For Connected Health Policy, Apr. 2016. Web. 24 Apr. 2017.
[10] LeRouge, Cynthia, and Monica J. Garfield. “Crossing the Telemedicine Chasm: Have the U.S. Barriers to Widespread Adoption of Telemedicine Been Significantly Reduced? .” International Journal of Environmental Research and Public Health 10.12 (2013): 6472–6484. PMC. Web. 19 Apr. 2017.